Addressing Melasma: Why the 1927nm Wavelength is Safer for Pigmentation in Skin Types IV-VI
Executive Summary :
Treating melasma in Fitzpatrick Skin Types IV-VI presents a profound clinical challenge due to the exceptionally high risk of Post-Inflammatory Hyperpigmentation (PIH). Traditional energy-based devices often trigger a reactive melanogenesis cascade by inadvertently overstimulating hyperactive melanocytes through excessive heat or acoustic shock. The 1927nm Thulium wavelength offers a statistically significant safety advantage by utilizing water, rather than melanin, as its primary chromophore. This non-ablative fractional photothermolysis mechanism limits thermal injury strictly to the epidermis (200-300 μm), precisely targeting the basal layer where pigment resides. By encapsulating melanin within Microscopic Epidermal Necrotic Debris (MENDs) for natural exfoliation, the 1927nm wavelength effectively eradicates pigment without triggering the inflammatory pathways associated with macrophage-mediated clearance. For aesthetic clinics, integrating this wavelength mitigates adverse event risks and establishes a highly predictable, ROI-driven protocol for complex pigmentary disorders in skin of color.
Executive Summary
- The PIH Dilemma in Skin of Color: Melasma treatment in Fitzpatrick Skin Types IV-VI is frequently complicated by reactive melanocyte behavior. Aggressive modalities often lead to rebound pigmentation or severe PIH, making thermal and acoustic control the absolute priority.
- Physics of the 1927nm Wavelength: Characterized by a high absorption coefficient for water, the 1927nm Thulium laser bypasses direct melanin targeting. This non-selective optical physics prevents the direct excitation of melanocytes, fundamentally lowering the risk of thermal aggravation.
- Targeted Epidermal Clearance: With an exact penetration depth of 200-300 μm, the energy is completely localized to the epidermis and the epidermal-dermal junction (EDJ), perfectly aligning with the anatomical location of epidermal melasma.
- Clinical and Commercial Value: By enabling the safe clearance of pigment without significant inflammation, the 1927nm wavelength empowers clinics to confidently treat darker skin tones, expanding their addressable patient demographic while ensuring robust clinical safety and an optimized return on investment (ROI).
The Clinical Challenge: Melasma and Fitzpatrick Skin Types IV-VI
Melasma is a chronic, acquired hypermelanosis characterized by symmetric, hyperpigmented macules and patches. While it affects all demographics, managing this condition in patients with darker skin tones requires a highly specialized approach.
Pathophysiology of Melasma in Skin of Color
In Fitzpatrick Skin Types IV-VI, the melanocytes are not necessarily more numerous, but they are inherently more biologically active, larger, and produce greater quantities of eumelanin. The pathophysiology of melasma involves not just the hyperproliferation of these melanocytes, but a complex interaction involving chronic ultraviolet exposure, hormonal fluctuations, and genetic predisposition.
Furthermore, patients with melasma often exhibit pathology at the Epidermal-Dermal Junction (EDJ). A compromised EDJ allows melanin and active melanocytes to drop into the upper dermis, complicating the clinical picture. Because the melanocytes in Skin of Color (SOC) are existing in a state of baseline hyper-responsiveness, treating them is often described by dermatologists as a “laser minefield.” Any sudden traumatic energy—whether excessive heat from continuous-wave lasers or aggressive acoustic shockwaves—can instantly trigger a defensive melanogenesis cascade.
The Risk of Post-Inflammatory Hyperpigmentation (PIH)
The most significant barrier to treating melasma in darker skin types is the onset of Post-Inflammatory Hyperpigmentation (PIH). Traditional light and laser therapies often rely on direct, aggressive targeting of melanin. When these modalities deliver high peak power or unmitigated bulk heating, they cause cellular rupture and significant localized inflammation.
This inflammatory cascade releases cytokines, arachidonic acid metabolites, and prostaglandins, which subsequently stimulate melanocytes to synthesize excess melanin as a protective physiological response. In severe cases of overtreatment, melanocyte destruction can lead to permanent hypopigmentation (confetti-like white spots). Therefore, the absolute core tenet of treating Fitzpatrick IV-VI is strict thermal control. The ideal modality must remove existing pigment while remaining entirely “invisible” to the hyperactive melanocytes, preventing the initiation of the inflammatory response.
The Optical Physics of the 1927nm Thulium Wavelength
To circumvent the risks associated with traditional pigment-targeting lasers, modern aesthetic medicine leverages the unique optical physics of the Thulium medium.
Chromophore Targeting: The Role of Water Absorption
The fundamental differentiator of the 1927nm wavelength is its chromophore affinity. Unlike Q-switched Nd:YAG or Ruby lasers, which are highly absorbed by melanin, the 1927nm wavelength’s primary target is interstitial and intracellular water.
Because water is uniformly distributed throughout the epidermal tissue, the 1927nm laser creates a uniform, non-selective thermal profile. It heats the tissue containing the pigment, rather than heating the pigment itself. By avoiding the direct photothermal or photoacoustic destruction of melanosomes, the 1927nm wavelength effectively “bypasses” the melanocyte’s alarm system. The melanocytes are not shocked into a defensive posture, which is the primary mechanism by which the 1927nm wavelength drastically mitigates the risk of PIH.
Precise Epidermal Penetration (200-300 μm)
Optical physics dictates that as the wavelength’s absorption coefficient for water increases, its tissue penetration depth decreases. The 1927nm wavelength possesses a higher water absorption rate than the 1550nm wavelength but lower than the 2940nm Er:YAG.
This specific absorption profile translates to a highly controlled penetration depth of exactly 200 to 300 micrometers (μm). This depth is clinically profound: it encompasses the entire epidermis and halts precisely at the superficial papillary dermis. Because epidermal melasma and the active melanocytes reside at the basal layer (the stratum basale) directly above the EDJ, the 1927nm wavelength delivers its thermal energy exactly where the pathology exists. It provides a “precision strike” that comprehensively clears epidermal pigment without delivering unnecessary and potentially inflammatory thermal bulk to the deeper dermal tissue.
Mechanism of Action: Eradicating Pigment Without Inflammation
The efficacy of the 1927nm wavelength relies on the principles of Fractional Photothermolysis, a mechanism that reorganizes tissue architecture safely and predictably.
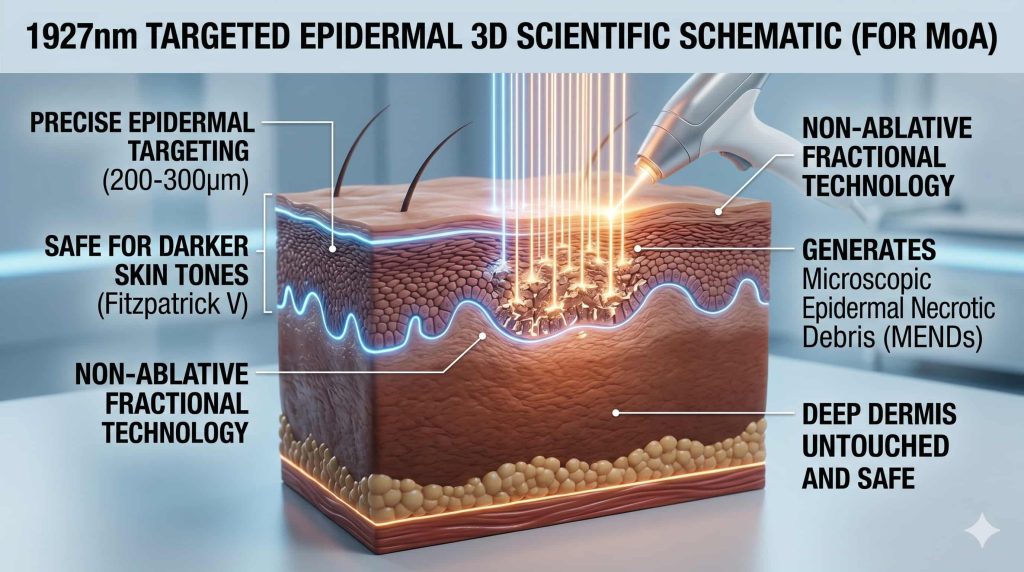
Formation of Microscopic Epidermal Necrotic Debris (MENDs)
As a non-ablative fractional laser, the 1927nm system does not vaporize tissue. Instead, it creates thousands of microscopic columns of thermal coagulation known as Microthermal Zones (MTZs). Within these coagulated zones, the pigment-laden keratinocytes are thermally denatured.
The body responds to this controlled thermal injury by rapidly extruding the coagulated tissue upward. The denatured cells, containing the trapped melasma pigment, form Microscopic Epidermal Necrotic Debris (MENDs). Over the course of 5 to 7 days, these MENDs migrate to the surface of the skin and are naturally exfoliated off. This process is often referred to in clinical literature as the “Sponge Effect.”
Crucially, this mechanism bypasses the need for macrophage-mediated phagocytosis. In traditional tattoo or deep pigment removal, lasers shatter pigment, relying on the immune system (macrophages) to digest and clear the debris—a highly inflammatory process. The 1927nm laser forces the pigment out through the epidermal barrier, clearing the melasma quietly and without triggering systemic localized inflammation.
Stratum Corneum Preservation
A critical safety feature of the 1927nm non-ablative approach is the absolute preservation of the stratum corneum. Because the optical energy coagulates rather than ablates, the outermost layer of the skin remains structurally intact.
This intact stratum corneum acts as a natural, biological dressing. It minimizes Transepidermal Water Loss (TEWL), preventing clinical dehydration of the treated area, and acts as a barrier against environmental pathogens, bringing the infection risk near zero. For B2B stakeholders and clinic operators, this translates to minimal patient downtime, higher patient compliance, and a drastically reduced post-operative complication rate.
Comparative Clinical Analysis: 1927nm vs. Traditional Modalities
For aesthetic practice owners evaluating capital equipment purchases, understanding how the 1927nm wavelength compares to legacy technologies is critical for establishing evidence-based protocols.
1927nm Thulium vs. 1064nm Q-Switched Nd:YAG
The 1064nm Q-Switched (QS) Nd:YAG has long been considered the gold standard for laser toning. Laser toning uses sub-thermolytic fluences to gradually suppress melanogenesis and break down pigment via the photoacoustic effect.
However, long-term clinical data indicates significant limitations. Prolonged and frequent sessions of 1064nm laser toning can lead to cumulative melanocyte toxicity, eventually causing refractory rebound melasma or irreversible mottled hypopigmentation. The 1927nm wavelength, conversely, offers structural tissue renewal. It actively removes the pigment via MENDs rather than merely suppressing it, requiring fewer sessions and offering a more stable, long-term clearance of the epidermal pathology without risking melanocyte death.
1927nm vs. IPL (Intense Pulsed Light)
Intense Pulsed Light (IPL) utilizes a broad spectrum of light (typically 500-1200nm) and relies heavily on high contrast between the target (pigment) and the surrounding tissue.
For Fitzpatrick Skin Types I-III, IPL is an efficient tool. However, for Skin Types IV-VI, IPL is inherently dangerous. The abundance of epidermal melanin in darker skin acts as a competitive chromophore, absorbing the broad-spectrum energy at the surface. This leads to catastrophic epidermal heating, resulting in severe burns, blistering, and profound PIH. The 1927nm laser’s reliance on water absorption completely bypasses this melanin-competition issue, making it statistically superior and vastly safer for skin of color.
Clinical Modality Comparison
| Parameter | 1927nm Thulium (NAFP) | 1064nm QS Nd:YAG (Toning) | Intense Pulsed Light (IPL) |
| Primary Chromophore | Water | Melanin | Melanin & Hemoglobin |
| Action Mechanism | Fractional Photothermolysis | Photoacoustic / Sub-thermolytic | Bulk Photothermal |
| Depth of Penetration | Epidermal (200-300 μm) | Deep Dermal (up to 4-6 mm) | Variable (Superficial to Mid-Dermis) |
| Risk of PIH in Types IV-VI | Very Low | Moderate to High (with cumulative use) | Extremely High (Contraindicated) |
| Risk of Hypopigmentation | Low | High (cumulative toxicity) | Moderate |
| Pigment Clearance Route | Epidermal Exfoliation (MENDs) | Macrophage Phagocytosis | Epidermal Exfoliation |
| Typical Downtime | 3-5 Days (Mild Erythema/Flaking) | Zero to Minimal | 7-10 Days (Crusting) |
Elevating Melasma Protocols with Cocoon Laser’s Advanced Technology
Transitioning from theoretical physics to clinical execution requires hardware that can deliver exact specifications reliably. As a premier aesthetic laser supplier, understanding the nuances of device engineering is paramount.
The Lav Dual Integration (1927nm Capabilities)
The integration of the 1927nm wavelength reaches its pinnacle in the Lav Dual system, engineered by Cocoon Laser. This advanced non-ablative fractional laser platform provides practitioners with unprecedented control over dosimetric parameters.
Treating melasma requires extreme precision; standard, inflexible parameters often lead to sub-optimal outcomes. The Lav Dual allows for granular adjustment of fractional density (MTZs/cm²), pulse duration, and power output. This means a dermatologist can customize the exact volume of tissue coagulation based on the specific Fitzpatrick phenotype and the severity of the melasma. Furthermore, the system incorporates advanced TEC Cooling (Thermoelectric cooling) at the handpiece interface. This continuous contact cooling protects the epidermis from transient heat spikes, maintaining a comfortable patient experience while virtually eliminating the risk of iatrogenic thermal injury.
Maximizing ROI for Aesthetic Practices
From a B2B procurement perspective, the Total Cost of Ownership (TCO) and the Return on Investment (ROI) are the ultimate drivers of capital equipment acquisition. Relying on legacy Q-switched or IPL systems limits a clinic’s ability to safely treat the growing demographic of patients with darker skin tones.
Integrating professional medical laser systems like the Lav Dual transforms a clinic’s operational capabilities. By establishing a reputation for safely and effectively resolving melasma in Fitzpatrick IV-VI profiles, clinics can capture a highly motivated and historically underserved patient base. The consumable model (such as the cost per shots count or roller tip) is engineered to maintain high profit margins per treatment session. Furthermore, the device’s robust build quality, backed by stringent medical certifications (such as Medical CE compliance), ensures continuous operational uptime, low maintenance overhead, and a rapid amortization schedule for practice owners.
FAQ: 1927nm Laser for Melasma in Darker Skin Tones
Q1: Does the 1927nm laser cure melasma permanently?
Melasma is clinically categorized as a chronic, hormonally and genetically influenced condition. There is currently no definitive “cure” for melasma across any medical modality. The 1927nm laser represents a highly effective management and clearance tool. It provides prolonged remissions by structurally clearing epidermal pigment safely. However, maintenance therapy, rigorous sun protection, and ongoing medical management are necessary to prevent long-term recurrence.
Q2: How many 1927nm sessions are required for Skin Type V?
For patients with Fitzpatrick Skin Type V, the clinical protocol demands a conservative approach to ensure absolute thermal safety. While lighter skin types might require 2-3 aggressive sessions, Skin Type V protocols typically recommend 4 to 6 sessions, spaced 3 to 4 weeks apart. This utilizes lower fractional densities and fluences to gently lift the pigment without exceeding the thermal threshold that triggers PIH.
Q3: Can 1927nm be combined with topical tranexamic acid?
Yes, and this represents the vanguard of modern melasma protocols. The fractional channels (MTZs) created by the 1927nm laser significantly enhance the permeability of the stratum corneum. Applying topical tyrosinase inhibitors, such as Tranexamic Acid or Vitamin C, immediately post-treatment leverages these micro-channels for deep transdermal delivery (Laser-Assisted Drug Delivery or LADD). This synergistic approach simultaneously clears existing pigment mechanically while suppressing new melanin synthesis chemically.
Q4: Where can clinics acquire certified 1927nm laser systems?
Procuring high-end aesthetic technology requires partnering with established manufacturers that provide robust clinical training, comprehensive warranties, and international regulatory compliance. Clinics seeking to integrate the 1927nm technology, specifically the highly customizable Lav Dual system, should initiate a direct consultation via the official inquiry portal at Cocoon Laser to discuss regional distribution, customized B2B pricing, and technical specifications.
If you need more information, please click “Contact Us”.
If you want to obtain more information, please follow our official website and Facebook.