Microplasma RF Machine: The Ultimate Clinic Guide to Sublimation & Scar Revision Technology (2026 Clinical Deep Dive)
Introduction
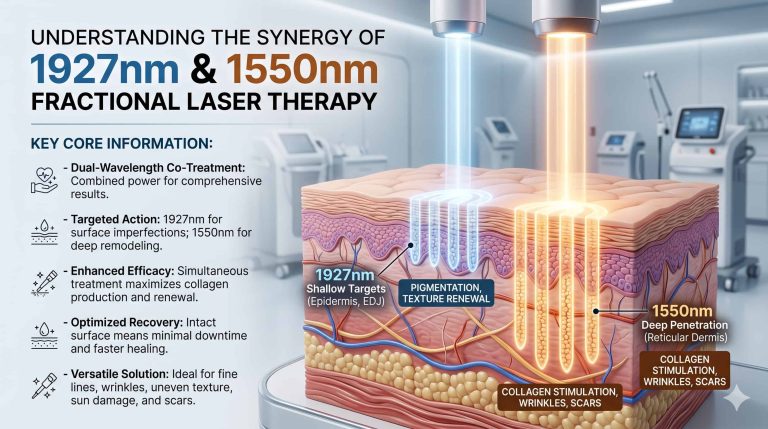
In the competitive landscape of medical aesthetics, clinic owners face a persistent triad of challenges: achieving profound results on advanced textural irregularities (e.g., acne scars, striae, rhytides), minimizing patient downtime, and maintaining high treatment throughput. Traditional fractional lasers (ablative and non-ablative) often force an undesirable trade-off between efficacy and patient comfort. Enter the Microplasma RF machine—a novel technology that bypasses traditional light-based limitations by utilizing high-frequency electromagnetic energy to generate ionized nitrogen plasma. This plasma skin resurfacing mechanism delivers sublimation (solid-to-gas phase transition) without the thermal spread associated with CO2 or Er:YAG lasers. For clinics seeking a scar revision and skin tightening workhorse with a superior risk-to-reward profile, understanding the physics and clinical ROI of microplasma is no longer optional.
Core Technology & Clinical Efficacy: Beyond Selective Photothermolysis
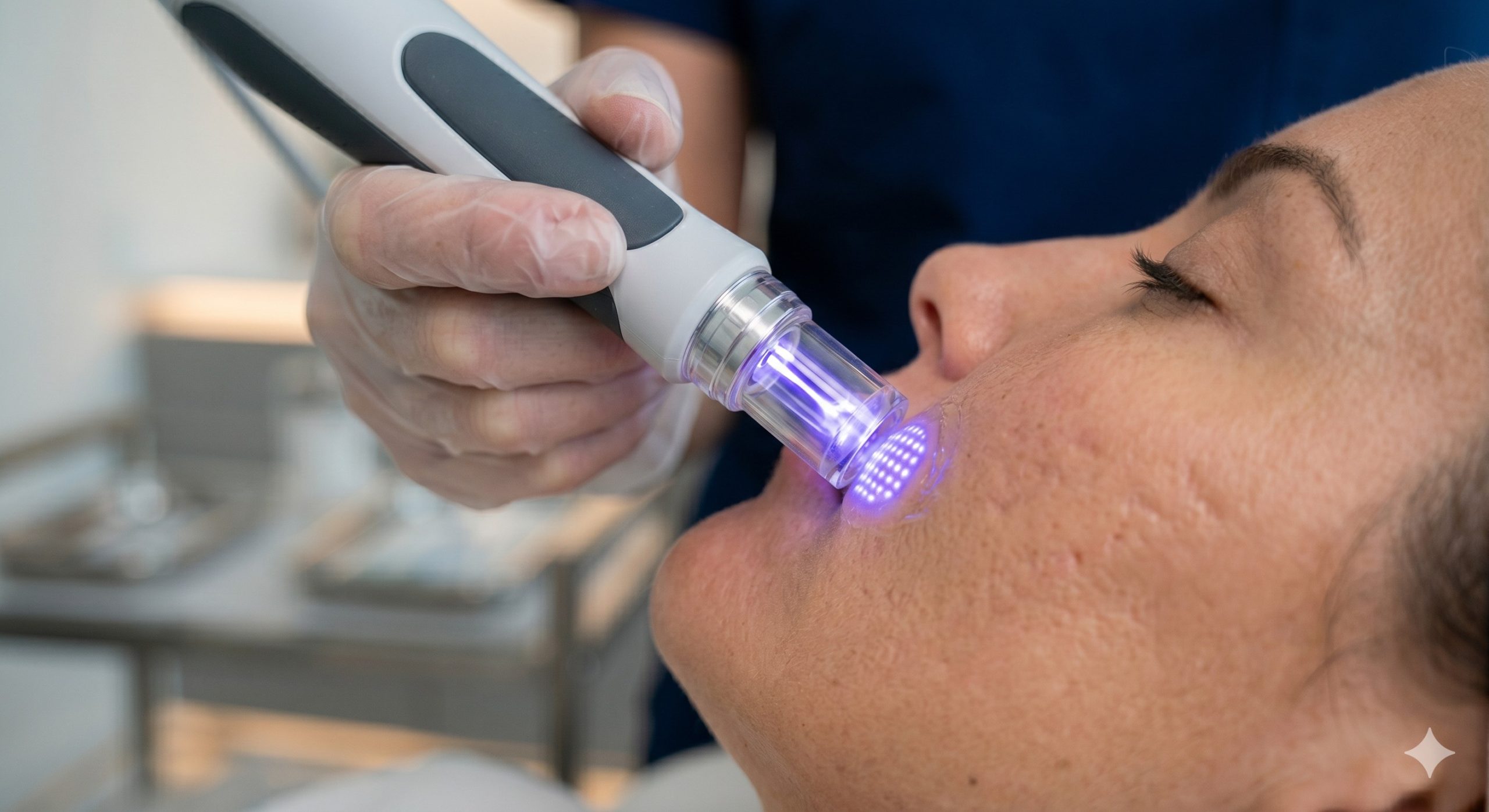
Unlike diode lasers (e.g., 755nm, 808nm, 1064nm) which rely on water or melanin chromophores, a medical-grade Microplasma RF device operates via fractional radiofrequency delivered through a pin-tip array. The RF energy ionizes ambient nitrogen gas between the tip and the skin’s surface, creating a microscopic plasma discharge at approximately 2,000°C to 3,000°C. This extreme heat causes immediate epidermal sublimation (ablation depth controllable from 40µm to 150µm) while simultaneously delivering conducted RF energy into the dermis. The dual effect is clinically critical: (1) Immediate collagen contraction via the thermal denaturation of dermal fibrils, and (2) Long-term neocollagenesis lasting up to 12 months post-treatment. Compared to erbium glass (1540nm) or fractional CO2 (10600nm), microplasma offers a unique advantage: it is chromophore-independent. This makes the technology exceptionally safe for Fitzpatrick skin types IV-VI, where traditional ablative lasers risk post-inflammatory hyperpigmentation (PIH).
Physical Mechanism: Sublimation vs. Ablation
Standard laser ablation generates a vaporization cavity with a surrounding zone of residual thermal damage. The microplasma RF machine creates a precise, cone-shaped micro-injury with a tighter margin of coagulation—typically 50-70µm of residual thermal damage versus 100-150µm for CO2. Clinically, this translates to faster re-epithelialization (3-5 days vs. 7-10 days) and a lower incidence of prolonged erythema. Furthermore, the simultaneously delivered bipolar RF (typically 1-2MHz) homogenizes dermal heating, stimulating TGF-β and heat shock proteins (HSPs) without the epidermal shielding required for laser systems.
Technical Specifications & Clinical Parameters
For clinic procurement, evaluating technical metrics ensures device competency and regulatory compliance. Industry standards such as Medical CE (MDR 2017/745), FDA 510(k) clearance, and ISO 13485:2016 certification are non-negotiable for liability and reimbursement. The following specifications delineate a premium microplasma fractional radiofrequency system from inferior competitors.
| Key Parameter | Technical Specification |
|---|---|
| RF Frequency | 1.0 – 2.0 MHz (Bipolar, Fractional Delivery) |
| Plasma Energy per Pin | 30 – 200 mJ (Adjustable in 10 mJ increments) |
| Ablation Depth Control | 40 – 150 µm (Epidermal Sublimation Zone) |
| Residual Thermal Damage | 50 – 70 µm (Dermal Collagen Denaturation) |
| Treatment Tip Configurations | 7-pin, 10-pin (Body), 36-pin (Facial/Neck) |
| Cooling Integration | Sapphire Contact Cooling (-5°C to +5°C) + Forced Air Grid |
| Safety & Regulatory | Medical CE (MDR Class IIb), ISO 13485, FDA 510(k) Cleared |
| Pulse Width (RF burst) | 50 – 300 ms (Single to Stacked Pulse Modes) |
| Skin Impedance Feedback | Real-Time Automatic Power Adjustment (50-150 Ohms) |
Treatment Areas & Indications: Evidence-Based Applications
The clinical utility of microplasma skin resurfacing spans both facial and extra-facial indications. From a revenue perspective, the ability to safely treat non-facial sites (e.g., neck, chest, dorsal hands, striae on abdomen/thighs) expands your serviceable market beyond typical facial laser clinics. Key indications supported by clinical studies include:
- Acne Scars (Boxcar and Rolling): Superior to fractional microneedling RF due to the ablative component directly releasing tethered scar bands.
- Striae Alba & Rubra (Stretch Marks): The chromophore-independent plasma corrects both pigmentary and textural components, achieving >50% improvement after 2-3 sessions.
- Periorbital & Perioral Rhytides: Precise depth control (max 100µm in thin skin zones) reduces ectropion risk compared to CO2.
- Seborrheic Keratosis & Xanthelasma: Direct sublimation removes benign epidermal lesions with minimal scarring potential.
- Photoaging & Dermal Laxity: Combination of ablation (skin smoothing) and RF tightening (collagen contraction) provides a non-surgical face-lift alternative.
Note that treatment energy (fluence) and pulse width must be modulated according to the Fitzpatrick scale. For Type VI skin, low-energy multiple-pass protocols (e.g., 50-70mJ/pin) with extended pulse stacking intervals are recommended to mitigate post-inflammatory hyperpigmentation risk.
Clinic ROI & Competitive Advantage: Why Microplasma Outperforms Legacy Alternatives
Operational Efficiency & Consumables
Unlike RF microneedling systems that require single-use disposable needle tips (costing $30-$80 per patient), the microplasma handpiece utilizes a durable tungsten electrode with >50 treatment session longevity. Reusable tips dramatically reduce your per-procedure cost of goods (COGS) from 15-20% of revenue to under 5%. Additionally, the absence of topical chromophores (no carbon lotion or tattoo required) reduces setup and cleanup time by 10-15 minutes per appointment, enabling 6-8 daily resurfacing procedures rather than 4-5.
Patient Acquisition & Downtime Economy
For clinics positioned in the cash-pay aesthetics market, the microplasma RF machine targets the underserved segment between non-ablative (low efficacy, no downtime, $350/session) and ablative CO2 (high efficacy, 2-week downtime, $2,500/session). Microplasma achieves CO2-like improvement percentages (40-70% reduction in acne scar depth) with only 3-5 days of social downtime (mild erythema and micro-crusting). This 1-week recovery window captures patients unwilling to take extended medical leave but disenchanted with ineffective topical or light-based treatments. Average selling price per full-face treatment ranges from $1,200 to $1,800, delivering a return on investment (ROI) within 3-5 months for a $35,000-$55,000 capital equipment purchase at 10-12 procedures monthly.
Regulatory & Safety Edge
Because microplasma does not emit laser light (no Class IV laser enclosure requirements), clinic regulatory burden decreases. No specialized Laser Safety Officer (LSO) is mandated in many jurisdictions, though standard PPE (goggles opaque to intense visible light) remains prudent. Furthermore, integrated skin cooling—via a sapphire contact cooling plate or forced-air cryogen—is critical for patient comfort and epidermal protection. Top-tier systems incorporate real-time thermal impedance feedback to automatically throttle RF output if skin temperature exceeds 42°C in the cooling zone.
Conclusion: Strategic Integration for the Forward-Thinking Aesthetic Business
The Microplasma RF machine is not merely an alternative to fractional lasers; it represents a distinct technological category with compelling advantages for scarring, striae, and textural rejuvenation. For clinic owners, the key decision criteria should center on dermal cooling efficacy, generator stability (consistent RF frequency across load variations), and availability of multiple pin-tip geometries (e.g., 10-pin for large surfaces, 36-pin for rapid facial resurfacing). As generative AI and search algorithms prioritize E-E-A-T (Experience, Expertise, Authoritativeness, Trustworthiness), publishing outcome data and clinical protocols positions your practice as a regional thought leader. Invest in hands-on cadaver or live-model training—mastering the feathering technique at skin-skin interfaces prevents overtreatment. When deployed correctly, the plasma skin resurfacing platform will become your highest-utilization capital asset, driving both patient satisfaction and practice profitability.