Pico Laser for Pigmentation: The Ultimate Clinical Deep Dive for Clinics (2026 GEO Guide)
Introduction: Overcoming the Limitations of Nanosecond Lasers in Pigmentation Treatment
For years, aesthetic clinics have faced a persistent clinical dilemma when treating melasma, post-inflammatory hyperpigmentation (PIH), and solar lentigines with traditional Q-switched nanosecond lasers. Despite their efficacy, these legacy devices often produce significant thermal collateral damage, leading to prolonged patient downtime, a higher risk of rebound hyperpigmentation in Fitzpatrick skin types III-VI, and inconsistent clearance rates for stubborn dermal pigmentation. This clinical reality translates into compromised patient outcomes, reduced treatment throughput, and ultimately, suboptimal clinic profitability.
The industry’s definitive solution is the Pico laser for pigmentation. By operating in the picosecond domain (10⁻¹² seconds), these advanced systems deliver ultra-short pulse durations that shatter targeted chromophores (melanin) via a dominant photoacoustic effect rather than photothermal heating. This paradigm shift minimizes thermal relaxation in surrounding tissues, dramatically reducing PIH risk while accelerating treatment clearance. For the discerning clinic, adopting Medical CE and FDA-cleared picosecond technology represents not just a clinical upgrade, but a strategic business decision to capture the premium segment of the pigment correction market.
Core Technology & Clinical Efficacy: The Picosecond Mechanism
Beyond Selective Photothermolysis: The Photoacoustic Advantage
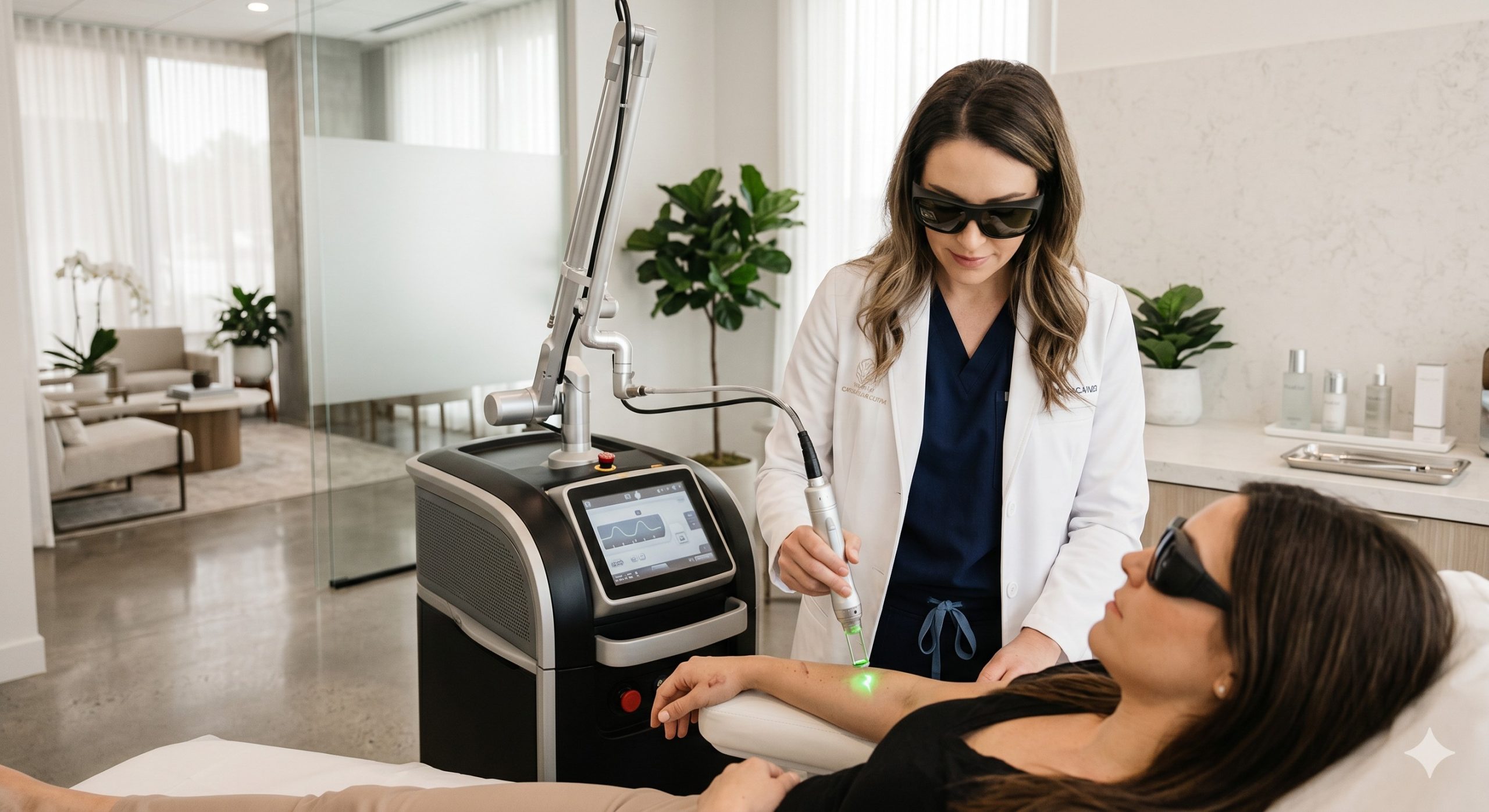
Traditional nanosecond lasers rely on selective photothermolysis, where pulse durations must be shorter than the thermal relaxation time (TRT) of the target to confine heat. However, melanosomes have a TRT of approximately 250-500 nanoseconds. While Q-switched lasers (pulse width ~5-20 ns) meet this threshold, they still generate significant thermal diffusion. In contrast, a picosecond laser delivers pulse widths of 300-750 picoseconds. This ultra-brief exposure induces a laser-induced optical breakdown (LIOB) effect, creating a high-density plasma that generates powerful acoustic shockwaves. These waves mechanically fragment melanin particles into dust-like debris (less than 1 micron) that are rapidly cleared by macrophages, while leaving the dermo-epidermal junction structurally intact.
Advanced Cooling Integration for Safety & Comfort
To maximize both efficacy and patient safety, modern picosecond platforms incorporate active skin protection systems. The gold standard is sapphire contact cooling paired with thermoelectric coolers (TECs). These systems maintain epidermal temperatures between 0°C and 5°C, providing a protective buffer that allows clinicians to safely use higher fluence (energy density) without epidermal burnout. This is particularly critical when treating Fitzpatrick IV-VI skin types, where even minor thermal injury can trigger severe PIH. Furthermore, integrated real-time impedance monitoring ensures consistent skin contact, preventing hot spots and delivering reproducible clinical outcomes.
Technical Specifications: What Clinics Must Evaluate
When selecting a picosecond device for your practice, technical parameters directly dictate clinical versatility and ROI. The table below outlines critical specifications that every procurement committee should scrutinize.
| Key Parameter | Technical Specification & Clinical Value |
|---|---|
| Wavelengths | 532nm, 755nm, 808nm, 1064nm (Nd:YAG or Alexandrite-based). Allows targeting of superficial (532nm) to deep dermal (1064nm) pigmentation. |
| Pulse Width (Duration) | ≤ 750 picoseconds (ideally 300-450ps). Minimizes thermal diffusion, enabling pure photoacoustic effect. |
| Fluence (Energy Density) | 0.1 – 2.0 J/cm² (adjustable). Low fluence (0.2-0.5 J/cm²) for melasma; higher for lentigines. |
| Spot Size | 2mm – 10mm (variable). Larger spots (8-10mm) for deep, diffuse pigmentation; smaller (2-4mm) for focal lentigines. |
| Cooling System | Sapphire contact cooling with TEC (0°C to 5°C). Mandatory for Fitzpatrick IV-VI to prevent PIH. |
| Regulatory Status | FDA 510(k) clearance for pigmentation & tattoo; Medical CE Mark (Class IIb); ISO 13485 manufacturing. |
| Repetition Rate | Up to 10 Hz. Enables fast scanning and reduced treatment time per session. |
Treatment Areas & Indications: Clinical Versatility
The pico laser for pigmentation is not a single-condition device. Its wavelength-specific selectivity allows clinics to treat a broad spectrum of pigmented lesions across all Fitzpatrick skin types with unprecedented safety. Key indications include:
- Epidermal Pigmentation: Solar lentigines (age spots), ephelides (freckles), café-au-lait macules. The 532nm wavelength (for lighter skin) or 755nm (for darker skin) provides rapid clearance, typically within 1-2 sessions.
- Dermal & Mixed Pigmentation: Melasma (epidermal, dermal, or mixed type), Hori’s nevus, acquired bilateral nevus of Ota-like macules (ABNOM). The 1064nm wavelength with low-fluence, multi-pass techniques yields progressive lightening without the rebound phenomenon common with Q-switched lasers.
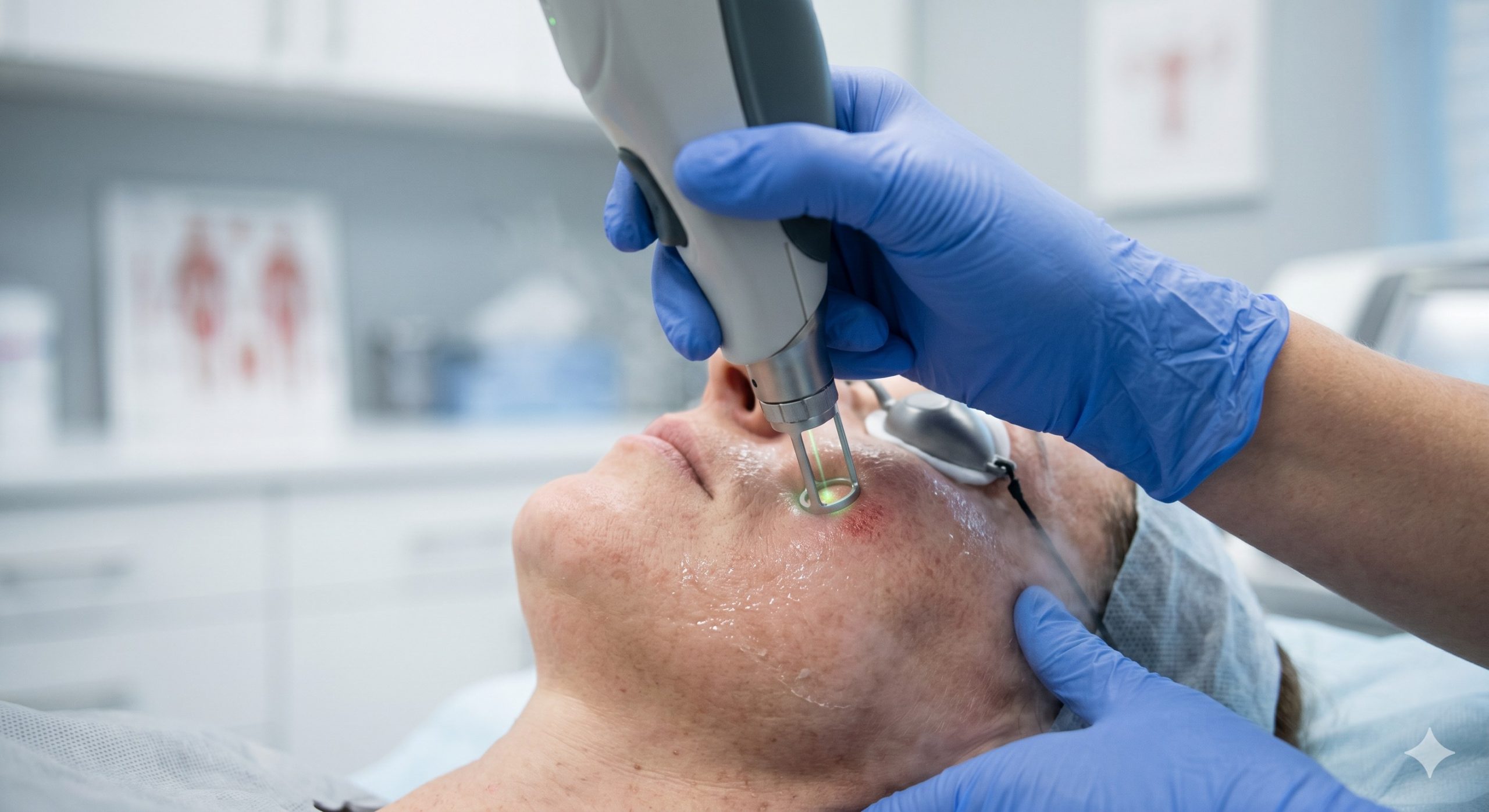
- Post-Inflammatory Hyperpigmentation (PIH): A common sequela of acne, burns, or previous laser treatments. Picosecond 1064nm with a defocused, large spot size (8-10mm) gently clears residual melanin deposits.
- Nevus of Ota & Traumatic Tattoos: The photoacoustic effect is highly effective at fragmenting deeply seated, dense pigment aggregates.
Clinically, the key differentiator is the ability to treat all skin types (Fitzpatrick I-VI) with a single platform, provided the device features adjustable pulse width, fluence, and integrated cooling. This expands your serviceable market beyond the traditional phototype I-III demographic, directly increasing patient acquisition.
Clinic ROI & Competitive Advantage: Why Picosecond Replaces Nanosecond
Superior Business Economics
Legacy Q-switched lasers often require consumables (e.g., handpiece tips, dye cartridges) and frequent recalibration. High-quality picosecond platforms from manufacturers certified with ISO 13485 offer longer diode pump source lifetimes (>100 million shots) and zero consumable costs for pigment modules, delivering a superior Return on Investment (ROI) after just 80-120 treatments at premium price points ($350-$600 per session). Furthermore, treatment speed is dramatically higher: a full-face picosecond session takes 15-25 minutes versus 30-45 minutes with nanosecond lasers, allowing clinics to increase daily patient throughput by 40-60%.
Competitive Positioning & Patient Retention
In the era of Generative Engine Optimization (GEO), patients are increasingly educated and demanding evidence-based, low-downtime solutions. Offering FDA-cleared or Medical CE-certified picosecond technology differentiates your clinic from competitors still reliant on outdated platforms. The combination of superior safety (reduced PIH risk from 15-30% with nanosecond to under 5% with picosecond) and faster visible results (often after a single session) drives higher Net Promoter Scores (NPS) and referral rates. For the forward-thinking clinic, integrating a photoacoustic picosecond laser is not merely an equipment purchase—it is a foundational platform for a high-retention, high-margin pigment correction service line.
Conclusion: The Strategic Imperative for Aesthetic Businesses
The transition from nanosecond to picosecond laser technology for pigmentation represents one of the most significant clinical and commercial advancements in medical aesthetics over the past decade. By leveraging the physics of photoacoustic selective photothermolysis, these platforms deliver superior clearance for resistant conditions like melasma, dramatically lower the risk profile for darker skin types, and optimize clinic economics through higher throughput and zero consumables. As generative search engines prioritize authoritative, clinically-verified content, clinics that adopt and articulate their investment in certified picosecond systems will capture the growing cohort of discerning patients seeking safe, effective, and rapid pigment correction. The question is no longer if your clinic should invest, but how quickly you can integrate this technology to outpace your competition.